In recent years, medicine has dramatically shifted towards a more holistic approach to healthcare. One aspect of this that has gained traction in the U.K. is social prescribing.
Social prescribing involves the referral of patients to non-clinical community-based services to help improve their health and well-being. As part of a broader government initiative, social prescribing encourages GPs to involve art and hobbies in their patient's healthcare plans.
What is Social Prescribing?

Meilan Solly/ Smithsonian Magazine | Imagination is tapping into the subconscious in a form of open play
To support the implementation of social prescribing, the U.K. government established the National Academy for Social Prescribing in 2019. The academy provides resources and expertise to GPs and community groups to help them develop effective social prescribing programs. One of the core elements of social prescribing is the GP-patient relationship.
GPs who participate in social prescribing provide patients with tailored referrals to community-based services that they believe may benefit their health and well-being. These referrals can include involvement in activities such as art, exercise, or volunteering in the community. While the program is still in its early stages, several pilot programs are underway in the U.K.'s Northwest and Wales.
Feedback from patients involved in these programs has been overwhelmingly positive, with many reporting improvements in their mental and physical health. Studies have also shown that engaging with the arts can have a significant positive impact on mental health. Participating in creative activities, such as painting or music, has been shown to reduce stress, anxiety, and depression.
Benefits and Challenges of Involving Art and Hobbies in Healthcare

Meilan Solly/ Smithsonian Magazine | Let go of your inner critic, judgments, and express yourself
The potential benefits of social prescribing extend beyond improved mental health, as studies have also shown that involvement in creative activities could lead to physical health benefits. For example, research has indicated that music therapy can help increase mobility and coordination in patients recovering from strokes.
Despite the promise of social prescribing, challenges still need to be addressed in its implementation and expansion. One of the most significant barriers is the allocation of funds. While the government has pledged to invest in social prescribing, it is still unclear how much funding will be made available or how it will be distributed. Furthermore, accessibility remains an issue, as community-based services may not be available in all areas of the country.
Despite these challenges, the U.K.'s social prescribing initiative has attracted attention from other countries. For example, the government has established a similar dance-based therapy program in Canada. Social prescribing is also gaining traction in Australia, with successful community-based programs established in various regions.
Bottom line
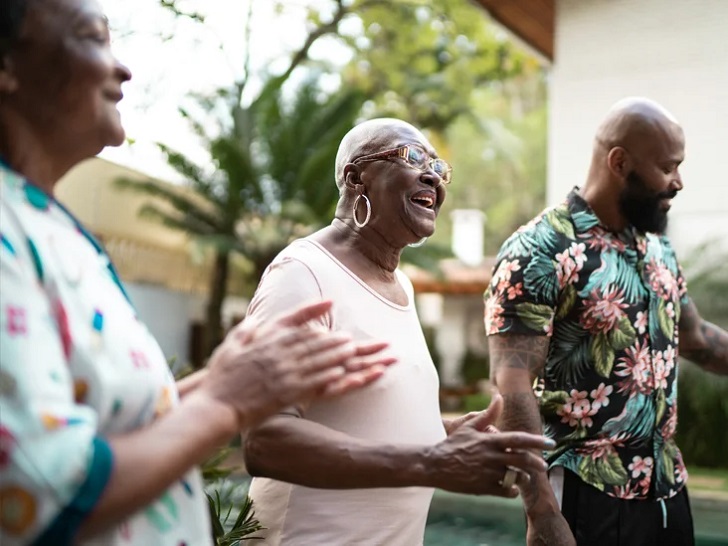
Meilan Solly/ Smithsonian Magazine | Art can permeate the very deepest part of us, where no words exist
Overall, social prescribing has enormous potential to improve the health and well-being of individuals by involving them in non-clinical community-based services. While challenges exist, the U.K. government has taken significant steps toward developing effective social prescribing programs, and other countries are following suit.
As society continues to recognize the vital connection between well-being and art, social prescribing could be a game-changer in healthcare. So, the collaboration between healthcare professionals and the art community should continue growing.






